Kidney Transplantation
A kidney transplant is a surgical procedure to place a healthy kidney from a living or deceased donor into a patient having irreversible advanced kidney disease (end-stage renal disease). Kidney transplant is considered to be the best treatment option as it can increase one’s life expectancy. Kidney transplantation is classified into deceased donor transplantation or living donor transplantation depending on the source of the donor organ.
Kidney (renal) transplantation is a surgical procedure in which a healthy kidney from a person (donor) is removed and placed in a patient (recipient) with irreversible advanced kidney disease (end-stage renal disease; ESRD).
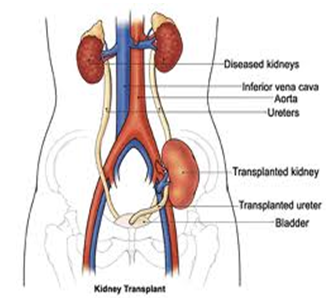
What is kidney transplantation?
Kidney (renal) transplantation is a surgical procedure in which a healthy kidney from a person (donor) is removed and placed in a patient (recipient) with irreversible advanced kidney disease (end-stage renal disease, ESRD).
Can I undergo living unrelated donor transplantation?
Living unrelated donor transplantation is not permitted by law, it is also unethical as it is associated with paid donation.
What are the types of kidney transplantations?
Kidney transplantation is classified into deceased donor transplantation or living donor transplantation depending on the source of the donor organ.
Who are the patients for whom transplantation cannot be done?
Patients with kidney disease that invariably recurs and damages the transplanted kidney (graft), recently diagnosed cancer, positive cross match (see below) and active infection cannot undergo transplantation.