Percutaneous Nephrolithotomy (PCNL)
Percutaneous Nephrolithotomy is a procedure used to remove kidney stones from the body when they can’t pass on their own. This is mostly used for larger stones or when other procedures, such as extracorporeal shock wave lithotripsy or ureteroscopy are unsuccessful or not possible.
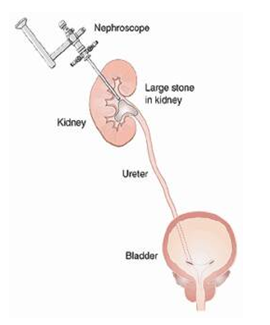
What is PCNL?
Initially cystoscopy is done. This involves passage of a thin, lighted, telescope through your urine passage, to see inside of the urethra and the bladder. Then a fine (ureteric) catheter is passed by the side of the stone into the kidney. This is used to inject contrast to visualize the details of the kidney during the PCNL.
Depending on the stone, renal anatomy and patient characterizes, your doctor may decide to do supine or prone PCNL. In supine PCNL, you will be lying on the back with little tilt to the other side, whereas in prone PCNL you will be lying on the stomach. In both the techniques, a 1 cm incision is made in the back, over the region of the kidney. Through this small incision, a track is made into the kidney to reach the stone. The entire process is guided by x-ray images. Whether it will be one single incision or more than one, depends upon the number of stones, their position, and the anatomy of the kidney itself. Once a track is established, an endoscope is passed into this track, and into the kidney to visualize the stone and remove it. Stones are broken by different methods. If the track is very small, stones are broken by laser.
Once the procedure is completed, a tube is left through this tract, as drainage, for one or two days.
What are the pre-operative tests that are required?
Apart from the routine blood and urine investigations, you will also need an ultrasound scan of the abdomen. An IVU (Intravenous Urogram) is a special X-rays to image the urinary tract or CT IVU (Computed Tomogram) will delineate the anatomy and function of the kidneys, helping to plan the appropriate treatment. Urine cultures are mandatory to detect and treat urinary infection, prior to the procedure.
Does this procedure need anaesthesia?
Yes, it is commonly performed under general anaesthesia and also therefore involves admission in the hospital.
What is the post operative course?
Generally you need to stay in the hospital for 3 to 4 days after the procedure. You will also undergo additional x-rays or ultrasound studies, to determine if there are any residual stone fragments present. Large amounts of residue will require the urologist to look again with an endoscope to remove them. The other alternative is to treat the remaining fragments with ESWL(Extracorporeal Shock Wave Lithotripsy) or RIRS (retrograde intrarenal surgery) with laser. In RIRS, the kidney stones are accessed from the urethra, bladder, ureter and then into the kidneys.
From the site of the puncture, you will have a drainage tube, which would be removed in a day or two. Following the removal of the flank drainage tube, urine may leak for a day. In some patients a ureteric stent (tube in your ureter), may be left indwelling. This stent would be removed by a small endoscopic procedure a couple of weeks later. Post-operatively your urologist will also encourage a high fluid intake, to keep the daily volume of urine produced to more than 2 litres a day. You will also be told to do deep breathing exercises.
When can I get back to work?
This would depend upon the magnitude of the stone burden and the number of tracts made. Most patients return to average activity levels within a week or so. A return to vigorous activity should probably take place after two weeks.
When should I come back after the procedure?
Your first review would be after two weeks. If you have a ureteric stent, it is usually removed then. You would also need a urine culture to check for any urinary tract infection. Further reviews will be advised by your doctor. You may be asked to get an X-ray or Ultrasound studies to document clearance of stones.
What is the main advantage of this approach?
Unlike traditional open surgery, only a 1 cm incision is made in the flank. The stones can be visualized directly and removed. The stones are removed in the same sitting and the kidney is cleared of calculi. The stay in the hospital is only for 3 – 4 days.
When would your doctor recommend this procedure?
This surgery would be recommended as a treatment of choice, if you have multiple kidney stones, larger than 2 cm kidney stones, bigger than 1 cm upper ureteric stones or at times the lower pole of the kidney which cannot be effectively treated with other methods like ureteroscopy (see below) or ESWL (Extracorporeal Shock Wave Lithotripsy). Renal stones which are considered very hard to break (having Hounsfield units greater than 1000 HU) are also preferably treated by PCNL.
This procedure is also performed following failure of other modalities of treatment such as medical therapy, ESWL, etc., for renal and upper ureteric stones.
What is the success rate of clearance of stones with this procedure?
It ranges between 90 to 95%. This actually depends upon the size, number and location of these stones. Sometimes if the operative time goes beyond 3 hours or there is pus in the kidney during puncture or there is bleeding causing drop in blood pressure, procedure would need to be stopped and in that case second procedure would be planned after 2-3 days. Small stone fragments may remain and they will usually pass out in due course of time.
What are the complications associated with this procedure?
By and large this procedure is safe. Some risks that can be associated with all surgical procedures are the possibility of bleeding (1%) sometimes requiring blood transfusion and infection.
Some patients have prolonged leakage of urine from the flank site, requiring ureteric stenting. Fever if present will require a change in antibiotic. Rare complications include persistent uncontrolled bleeding due to vascular conditions (0.4%), and this may require secondary procedures to stop bleeding by inserting coils to block the bleeding vessels by a vascular surgeon or even a nephrectomy to control the bleeding. When a puncture is made at the upper pole of kidney (above 12th rib), complications would then include entry of air or fluid or blood accumulation in the chest cavity. Again the incidence of these is only 0 – 4%. Rarely when the puncture is done through the lower pole of the kidney surrounding organs like large bowel or spleen or liver may be injured requiring additional surgical procedures.
What are the contraindications to this procedure?
These are bleeding disorders and pregnancy (due to risk of radiation). The others are medical problems making the patient unsuitable for anaesthesia.
How do you prevent recurrence of stones?
It is advisable to maintain a urine output of about 2 liters per day. Your doctor will give a similar brochure on dietary changes. Medications, if needed, would be based on stone analysis reports or later metabolic tests.