Regional anesthesia is anesthesia for the region where the surgeon is going to operate. This is done by injecting anesthetic drug near a cluster of nerves, numbing a larger area of the body (such as below the waist or one limb) so that the surgeon can operate on it without you feeling pain. You will not be unconscious but the affected area may feel heavy and numb. These effects are temporary and will wear off after the surgery.
What is regional anaesthesia ?
Regional anaesthesia is anaesthesia for the region where the surgeon is going to operate. This is done by injecting anaesthesia drug near a cluster of nerves, numbing a larger area of the body (such as below the waist or one limb) so that the surgeon can operate on it without you feeling pain. You will not be unconscious but the affected area may feel heavy and numb. These effects are temporary and will wear off after the surgery.
With regional anaesthesia, though you may remain awake, you may usually also be given a sedative to help calm you. Prior to administering the anaesthesia: Your doctor will set up monitors to track your vital signs. A local anaesthesia will be applied to the skin or injected to make even the injection of anaesthesia painless. Epidural and spinal are some of the examples of regional anaesthesia. Both involve injecting medicines in or near the spinal canal at levels selected by your anaesthetists.
How is the epidural block performed ?
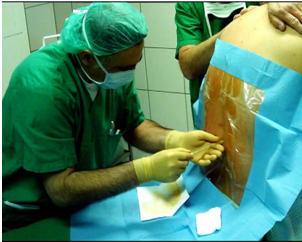
An epidural or spinal block is given in the back. You will either be sitting up or lying on your side. Before the block is performed, your skin will be cleansed with an antiseptic solution. The anaesthesiologist will use local anaesthesia to numb an area of your back.
For the epidural block, a needle is first placed in the epidural space just outside the spinal sac. A tiny flexible tube called an epidural catheter is inserted through this needle. Occasionally, the catheter will touch a nerve, causing a brief tingling sensation down one leg. Once the catheter is positioned properly, the needle is removed and the catheter is taped in place. Anaesthetic and additional medications are administered as needed through this epidural catheter, without repeated needle pricks. The medications bathe the nerves and blocks out the pain. This produces epidural anaesthesia and analgesia.
For the spinal block, a small needle is placed in spinal sac. Occasionally, the needle will touch a nerve, causing a brief tingling sensation down one leg. Once the needle is positioned properly, medication is administered. The medication bathes the nerves and blocks out the pain. This produces spinal anaesthesia and analgesia.
Will i get back pain after injection in the back ?
You may have some pain or discomfort in the low back region for a day or two because of lying down on the bed. But, you will not have pain in your back because of the spinal or epidural procedure.
Can the regional block used for my surgery also help with pain relief after surgery
The regional block used for the surgery may last for some time after the end of surgery and may help with pain relief during this time. Commonly the catheter used for epidural anaesthesia may be retained for couple of days post-operatively to extend the duration of pain relief after surgery.
What are the possible side effects from the medications used for pain relief after surgery ?
The two commonly used types of medications are opioids (narcotics) and local anaesthetics. In normal doses, narcotics may cause some itching, nausea, retching, or drowsiness. Local anaesthetics may cause some numbness or, heaviness. There will be some difficulty with weight-bearing on the blocked leg afterwards, and patients should take care not to fall; however, the pain control lasts longer than the motor effects.
What are the benifits of regional block ?
Frequently, there is less nausea from regional blocks and patients generally awaken faster after regional blocks. Regional blocks can also be used to reduce the pain after surgery. Generally, regional nerve blocks and catheter will provide better pain control than intravenous or intramuscular opioids (narcotics).
Epidural analgesia for pain control after surgery might provide you with some specific benefits:
Better pain control than intravenous narcotics
Earlier recovery of bowel function
Less need for systemic opioids (narcotics) and less nausea as a result
Easier breathing resulting from better pain control
Easier participation in physical activity
What is a spinal headache ?
A spinal or postdural puncture (PDPH) (or also sometimes called a meningeal puncture headache) may occur after spinal or epidural anaesthesia when puncture of the dural sac allows for spinal fluid to leak out of the dural sac. If enough spinal fluid leaks out, a headache may occur especially when standing or sitting. A spinal headache may occur any time after spinal or epidural anaesthesia but most cases generally show themselves within 3-5 days after a spinal or epidural anaesthetic. The characteristics and severity of the headache may vary. It is normally managed with simple measures like increasing fluid intake, bed rest and taking paracetamol tablets. With improvements in needle design, the risk of a spinal headache after anaesthesia is much less than a few decades ago. Most of the time it is self limiting and very rarely it will need inpatient treatment. The incidence of headache is 0.1% -1%.
What is difference between spinal and epidural anasthesia ?
Spinal anaesthesia and epidural anaesthesia both are given in the almost same place but spinal anaesthesia is a one-time injection lasts for 2-3 hrs and you will not be able to move your legs at all. Epidural anaesthesia can be either a one-time injection or can be continuously delivered through an indwelling epidural catheter, and usually does not result in complete paralysis of lower limbs.